What causes ARMD?
ARMD, generally occurs as a result of changes in the macula due to ageing.
Factors influencing the development of ARMD include:
- Age 50 years +
- Family history of ARMD/genetics
- Smoking
- High blood pressure
- Heart disease
- High cholesterol levels
- Excess weight
- High saturated fat diet (found in foods like meat, butter and cheese)
- Lack of exercise
- UV exposure.
What are the symptoms of macular degeneration/ARMD?
If you have dry ARMD in its early stages, you will have no pain or discomfort and the condition may be detected in an eye exam before you even experience any symptoms.
Symptoms include:
- Difficulty seeing fine detail in the centre of your vision – the size of the affected central area may increase
- Blurred vision
- Dark spots or missing areas of vision
- Distorted vision (straight lines appearing wavy)
- Numbers and letters appearing jumbled
- Words disappearing when reading
- Difficulty discerning colours and shades of colours
- Poor adaptation to dark conditions from lighter environments
- Requiring more light to perform daily tasks
- Difficulty reading that is not improved with new glasses
- Impaired depth perception – an inability to properly judge distances which can make walking harder and lead to falls.
Around 10 to 15 per cent of people with dry ARMD develop wet ARMD, so, if you have been diagnosed with dry ARMD and experience any sudden change in vision, you should see your eye care professional urgently as early detection is crucial. The earlier you seek treatment, the more likely you are to have a better outcome.
How is macular degeneration/ARMD diagnosed?
Everyone, particularly if you are aged 50+, should have regular eye examinations.
Your ophthalmologist will review your medical and family history and will conduct a variety of tests using photography or other imaging to examine your macula and detect early signs of ARMD. If you experience any of the symptoms listed above, you should make an appointment with your ophthalmologist as soon as possible.
Your ophthalmologist may use the ‘Amsler Grid’ (See below) in your diagnostic consultation and may recommend you regularly self-monitor any changes in your vision by using it. You should contact your ophthalmologist immediately if you notice that lines, or parts of the grid look wavy, blurry or dim.
The Amsler Grid
Normal Vision Distorted Vision
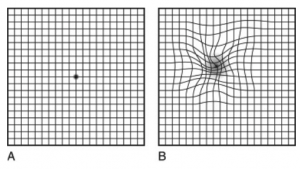
How is ARMD treated?
Wet ARMD
If detected early, wet ARMD can be treated, although not cured. The various treatments, which target the blood vessels that grow abnormally into the retina, include:
- Injections of drugs into your anaesthetised eye to stop growth of abnormal blood vessels
- Photodynamic therapy which is a combination of drug and laser treatment aimed at sealing leaky blood vessels
- Laser treatment which uses a light beam directed onto the retina to seal leaky blood vessels.
Your LEI ophthalmologist will discuss which treatment options are most appropriate for you.
Dry ARMD
Unfortunately, there are no medical treatments for dry ARMD. But a healthy lifestyle is important in reducing the risk of macular degeneration and in slowing its progression.
Smoking is the main modifiable risk factor for ARMD. Research has shown that the risk of developing ARMD is at least double in smokers than in non-smokers.
Other healthy habits to develop and continue include:
- Maintaining a healthy weight
- Eating a nutritious diet that includes green leafy vegetables, yellow and orange fruit, fish, and whole grains
- Maintaining normal blood pressure and controlling other medical conditions
- Exercising regularly
- Wearing sunglasses and hats outdoors
- Wearing lenses that block UV and blue light, and reduce glare.
- Having regular eye tests to spot problems.
Some eye specialists recommend vitamin supplements to reduce the progression of dry ARMD. It is best to discuss this directly with your ophthalmologist.
Download the fact sheet



