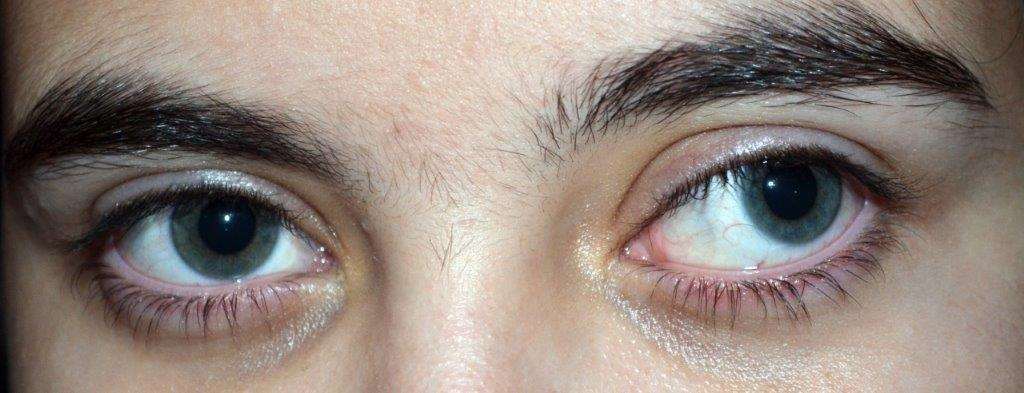
What is Strabismus?
Strabismus is the condition where the eyes are not properly aligned. Other common names include ‘lazy’, ‘crossed’ or ‘turned’ eyes, and ‘squint’.
One or both eyes may turn either inward (esotropia), outward (exotropia), upward (hypertropia) or downward (hypotropia).
Strabismus may be constant or intermittent and might always affect the same eye (unilateral), or both eyes may take turns in being misaligned (alternating).
Strabismus is the most common eye disorder in children. It’s estimated that between three and five per cent of Australians are affected by the condition.